Imaging the Knee
by Dr. Vinaya Kunjir
Radiologic investigations are the starting point for diagnosis and disease assessment of any joint pain. Here we are going to briefly discuss general aspects of knee joint imaging and in particular arthritis.
How is the knee joint formed
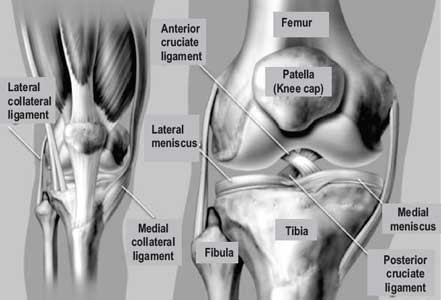
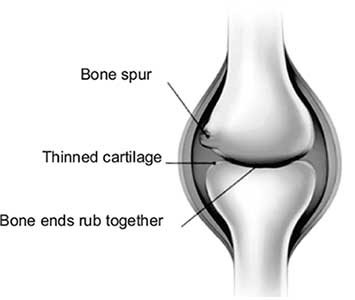
Knee joint is the complex synovial joint formed by thigh bone (femur), Tibia (bone in the leg) joined in front by smaller knee cap i.e. patella. Apart from these, smaller bone (fibula) is seen alongside tibia in the leg. The bony ends forming the joint are covered by the articular cartilages.
The bones forming the joint are supported by ligaments and menisci. These also help to regulate movement at the knee. Anterior cruciate (ACL) and posterior cruciate (PCL) ligaments as well as the medial collateral (MCL) and lateral collateral (LCL) ligaments provide stability to the joint and prevent sliding. C shaped medial and lateral menisci lie between femur and tibial articular surfaces and function as shock absorber.
Knee X RAY/ RADIOGRAPH
Common knee views taken are antero-posterior (AP), weight bearing PA, lateral (Lat) and skyline view.
The AP view is looking at knee held directly from the front. Weight bearing PA view is taken to detect early arthritis. The Lateral view is taken looking from the side perpendicular to the AP view. Skyline view is taken with knee in bent position and it assesses the joint between knee cap and femur.
Cartilage is not visible on X ray so even though the cartilage covered bone ends are in proximity to each other there appears to be a gap between them on X ray. The gap is nothing but the joint space; it is divided into medial and lateral compartments and is of uniform and even height in normal knee.
Imaging
Osteoarthritis of the knee is the most common degenerative disease affecting men and women. Knee is also a common joint to be affected in other rheumatic arthritis and acute & chronic infections
What do we see on X ray in Knee Arthritis?
Joint alignment and bone density
Joint space
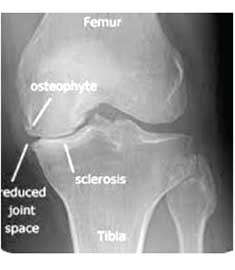
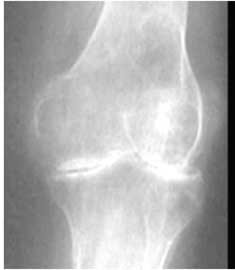
Joint space reduction which can involve entire joint or selectively involve only the medial compartment. It is an early indicator of the joint degeneration and inflammation.
Degenerative changes
Though cartilage is the most affected part, it cannot be directly seen on X ray. Osteophytes (bony outgrowths), Spiking of tibial spines are the prominent features seen on radiograph.


.jpg)